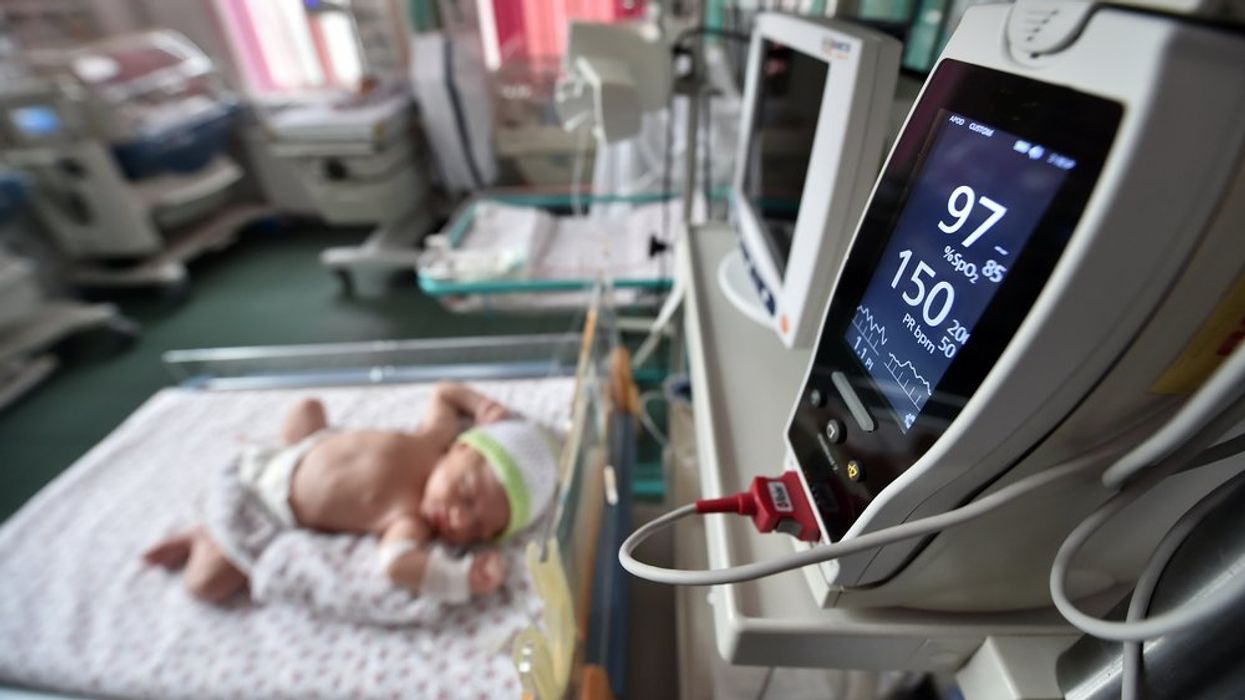
In the United States, one in 5,000 women die during childbirth, making it the most dangerous developed country to give birth in. For women in rural areas, the risk is even higher.
The American Hospital Association reported that from 2015 to 2019, around 90 hospitals in rural areas closed their obstetric units. In 2020, half of rural hospitals had stopped offering obstetrics care. The closures are expected to accelerate, as another study of hospital administrators before the Covid-19 pandemic found that 20 percent did not plan on offering labor and delivery services within five years.
A study in the National Library of Medicine also found that women in areas without care are three times as likely to die than those who have access to it, as critical services such as ambulances have greater struggle reaching them.
Lack of medical care particularly harms Indigenous communities, as they are more likely to live in rural areas. The risk of Native American women dying of pregnancy-related complications is three times higher than White women, with their babies twice as likely to die.
Women on the Yakama Indian Reservation in Toppenish, Washington experienced the abrupt closure of their only hospital's maternity unit. The decision was made without consulting the community, the doctors, or its own board, which the community expressed outrage at during a recent city council meeting.
“There will be lives lost — people need to know that,” said Native American doula Leslie Swan, via The New York Times.
“It’s a lifeline that we’ve had, and now that part of that lifeline is getting cut down,” Semone Dittentholer of the Ttawaxt Birth Justice Center added. “It’s just another reminder of how scary it can be out here.”
Increasing staffing shortages of labor and delivery nurses, as well as rising equipment costs, have put many hospitals in precarious situations. Cassie Sauer, president and chief executive of the Washington State Hospital Association, expects shortages to rise without aide.
“Toppenish is the canary in the coal mine,” she said.
- Homicides Against Pregnant Women Have Risen, Report Reveals ›
- 85 Percent of Rural California Are at High Risk of Wildfires ›
- It's Become Harder For Women to Access Reproductive Healthcare | AdvocateChannel.com ›
- Calls to End Violence Against Native Women Grow on 'Missing or Murdered Indigenous Persons Awareness Day' | AdvocateChannel.com ›